A Fight Worth Fighting For: Stage 3 Lung Cancer
Helen had never smoked. She had no symptoms. And yet in November 2022, she was diagnosed with stage 3 lung cancer — tumours occupying nearly half her lungs. Most would have called it incurable. Helen decided it was a fight worth having.
The Diagnosis
Helen had never smoked a day in her life. Nobody in her family did. So when a routine annual health screening at the end of October 2022 flagged a large white shadow on her left lung, it was the last thing she could have anticipated.
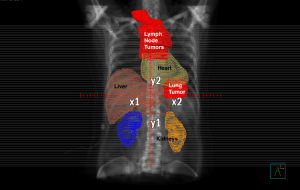
The blood tests, ultrasound, and treadmill test had all come back normal — it was the X-ray that raised the alarm. Her doctor advised a CT scan for a clearer picture. The results, received in November 2022, were shocking: three sizeable tumours measuring 6.2cm, 3.7cm, and 3.5cm, along with multiple smaller tumours in the lymph nodes. A biopsy confirmed it — a rare type of stage 3B lung cancer, still under active research. “It felt like my world collapsed. I couldn’t believe it. How could I have lung cancer? I’m a non-smoker. I really don’t like the smell of cigarettes. No one in my family smokes at all. Why did I develop lung cancer — and already at such an advanced stage, without any symptoms?”
What had made the diagnosis harder to catch was a two-year gap in screenings during the COVID-19 pandemic. By the time Helen returned for her check-up, the disease had already progressed silently. In her search for answers online, what she found only deepened the fear: no source suggested that advanced-stage lung cancer could be cured. Life expectancy, she read, was often no more than a year. It felt like a death sentence.
But Helen was not willing to accept that verdict without a fight. She had parents, a husband, siblings, and children who loved her. “I wasn’t willing to leave them without any fight, even though the verdict had already been given to me.”
The Journey
Her respiratory specialist confirmed that surgery was not an option. The first step would be chemotherapy — to destroy or inhibit the growth of cancer cells before any further intervention could be considered.
Helen began chemotherapy on 8 December 2022. After three sessions, a CT scan brought the first ray of hope: all three tumours had visibly shrunk. The largest had reduced from 6.2cm to 4.9cm, the second from 3.7cm to 2.2cm, and the third from 3.5cm to 1.9cm. After seven full sessions, a PET scan showed the main tumour continuing to reduce — and, crucially, there had been no spread.
However, the rate of tumour reduction had begun to slow, suggesting that the cancer cells were adapting to the drugs. Her oncologist recommended adding radiotherapy — to attack the remaining cancer cells more precisely and effectively. Helen was referred to Dr. David Tan and the team at AARO.
The Treatment
DR. DAVID TAN · RADIATION ONCOLOGIST, AARO
Helen’s cancer was very advanced even for a stage 3 diagnosis. She had a large primary tumour in the left lower lobe which had spread extensively to the central lymph nodes compartments in the mid-chest and even the compartments in the right upper lung. Essentially, the tumours had occupied almost 40-50% of her lungs and had already crossed from the left to the right side. Many experienced lung oncologists would consider this an incurable situation, because such extensive disease would firstly be difficult to treat aggressively without causing significant collateral damage to the surrounding organs, and secondly, experience has shown us that such cancers, even with an initial good response, would inevitably recur either in the same area or elsewhere in the body.
During our first consultation, I had a long and honest discussion with Helen and her family to explain the gravity of the situation. The first and most appropriate treatment option was then explained to them — palliative radiotherapy, where low doses of radiation are given over two to three weeks to control the existing tumours, possibly achieve some shrinkage, and to prevent symptoms from worsening. This option would also minimise side effects and provide good quality of life for her remaining life expectancy. However, Helen and her family found this option very difficult to accept. She wanted desperately to fight and to live on for her young children and her husband.
The alternative and more aggressive treatment approach was then discussed with the family. This option would involve high doses of daily radiation therapy concurrent with three-weekly chemotherapy, to be delivered over six weeks. Due to the large and irregular treatment field, we would also need to harness the latest technologies to tightly conform the radiotherapy doses around the treatment area. Even so, the radiotherapy would still carry the risk of significant toxicity due to the large treatment area and the much higher doses required to offer a chance of complete tumour eradication. Helen would have to brace herself for the side effects of treatment, and even the possibility of aborting treatment midway if the toxicities became too severe. After much deliberation with her family, Helen chose to proceed with this aggressive option.
Fighting Through
On 19 June 2023, Helen began her 30 sessions of radiotherapy, running in parallel with her final rounds of chemotherapy. The side effects accumulated — allergies, hair loss, bone pain, profound fatigue, a complete loss of taste, and as radiotherapy progressed, wounds that made swallowing almost impossible. During sessions 26 through 30, she came closest to her limit. She was hospitalised during this period due to physical weakness. And yet she completed every one of the 30 radiotherapy sessions — and all 11 rounds of chemotherapy. “I almost gave up. But my family, Dr. David and the medical team kept encouraging me. All of this became my greatest source of strength to keep going and not give up.”
Thriving After Cancer
31 July 2023. Helen’s final treatment.
“Gratitude, relief, and emotion all came together. I felt deeply moved because I was able to go through a process that was not easy — something that might even have seemed impossible — but I made it through and achieved victory.” She was grateful that she did not walk that road alone — Dr. David Tan and the team at AARO were with her through every difficult chapter, not only medically, but emotionally. “They always provided clear explanations, patiently answered my questions, and offered support at every stage of the treatment. Their presence made me feel that I was not alone in facing this cancer journey.”
Three months after completing treatment, Helen underwent a follow-up PET scan. The results were definitive: all tumours and cancer cells had disappeared.
Dr David recounted the remarkable outcome of Helen’s treatment – Helen’s first follow-up PET scan in November 2023 showed a complete metabolic and radiological response to treatment. The primary tumour in the left lower lung had disappeared, and the extensive lymph nodes in the central and right upper lung had all shrunk back to normal parameters. There were no new areas of disease elsewhere in the body.
“I have since been following up with Helen for her cancer surveillance over the past two and a half years. Her repeat scans, performed every four to six months, have remained clear with no evidence of recurrence. Helen also remains well, with no long-term side effects from her chemoradiotherapy. Her remarkable response and recovery stand as a testament to her determination and resilience in completing a gruelling course of treatment for the sake of those she loves. It is also a demonstration of how honest, collaborative discussion with the patient, coupled with diligent use of our latest cancer technologies, can make the difference between life and death.
I am glad to have played a role in Helen’s cancer journey, and cherish the heartwarming family photos she sends every now and then — reminders of the joys of family, and the power of love.”
—————-
Since her treatment, Helen have had the opportunity to share special moments with her family. “Moments that might not have been possible if I hadn’t gone for the treatment,” Helen says — and in those simple words lives the full weight of everything she endured, and everything she has gained.

She now wants to share her experience with others who are still in the middle of their fight — with the honesty of someone who has been there. She knows what it feels like to read statistics that offer no hope. And she is standing, smiling, as living proof that neither the statistics nor the fear gets the final word.
“The journey of fighting cancer is full of challenges, but it also brings many valuable lessons. I learned about strength, patience, and the importance of hope. I want to tell anyone who is still fighting: Never lose hope. Keep believing that there is always a way and always a chance to recover. Miracles are for those who believe in Him. Today I stand here as proof that miracles and hope are real.”
This season, we are honoured to celebrate our Ambassador of Hope: Helen.